Understanding Gynaecological Cancer Screening and Its Importance
Gynaecological Cancer screening plays a critical role in protecting women’s health by helping detect potential Cancers at an early stage. Many gynaecological Cancers develop silently, showing little or no symptoms in the initial phases. Screening allows abnormalities to be identified before they progress, offering women the opportunity for timely medical evaluation and appropriate management.
For women of all age groups, especially those above 30, regular gynaecological Screening is an important step toward long-term reproductive and overall health.
What Is Gynaecological Cancer Screening?

Gynaecological Cancer screening refers to a group of medical tests and evaluations used to detect early signs of Cancers affecting the female reproductive system. These screenings focus on identifying abnormal cellular changes, structural abnormalities, or risk indicators before Cancer becomes advanced.
Unlike diagnostic tests performed after symptoms appear, screening is often done when a woman feels healthy. The goal is early identification rather than treatment of advanced disease.
Types of Gynaecological Cancers Covered in Screening
Gynaecological Cancer Screening primarily focuses on Cancers that affect the female reproductive organs. These include Cancers of the cervix, ovaries, uterus, vagina, and vulva.
Among these, cervical, ovarian, and uterine Cancers are most commonly addressed through structured screening and evaluation. Each Cancer type requires a different screening approach, depending on how it develops and how early changes can be detected.
Why Early Screening Matters for Women’s Health
Early detection is the strongest advantage of gynaecological Cancer screening. When abnormalities are detected at an early stage, management options are usually simpler, less invasive, and associated with better outcomes.
Women who undergo regular screening are more likely to identify issues before symptoms become severe. This proactive approach reduces uncertainty, helps with informed decision-making, and supports long-term well-being.
Who Should Consider Gynaecological Cancer Screening?
Gynaecological Cancer screening is not limited to women who have symptoms. Many women without any noticeable signs benefit from screening, particularly those with certain risk factors.
Women may consider screening if they:
- Are above 30 years of age
- Have irregular menstrual bleeding
- Experience unexplained pelvic discomfort
- Have a family history of gynaecological Cancers
- Want preventive evaluation despite no symptoms
Screening recommendations are always individualised based on age, medical history, and risk profile.
Understanding Risk Factors in Gynaecological Cancers
Risk factors do not mean that Cancer will develop, but they can increase the likelihood of certain conditions. Understanding these factors helps women and healthcare providers decide when screening may be beneficial.
Common risk factors include increasing age, hormonal imbalance, obesity, smoking, family history, and long-term hormonal therapy. Identifying these factors early allows for timely screening and closer monitoring.
Screening vs Diagnostic Testing- Knowing the Difference
It is important to distinguish between screening tests and diagnostic tests. Screening tests are performed in women without symptoms to identify early changes. Diagnostic tests are used when symptoms or abnormal screening results are present.
Screening does not confirm Cancer; it highlights the need for further evaluation if abnormalities are detected. This step-wise approach prevents unnecessary anxiety while ensuring safety.
Psychological Benefits of Regular Screening
Apart from physical health benefits, regular gynaecological screening provides reassurance. Knowing that health is being monitored reduces stress and uncertainty for many women.
Clear communication, understanding the purpose of screening, and knowing what to expect helps women feel more confident and informed about their health decisions.
Importance of Individualized Screening Plans
There is no single screening schedule that applies to all women. Screening plans are tailored based on age, medical history, symptoms, and personal risk factors.
This individualised approach ensures that women receive appropriate evaluations without unnecessary tests.
Screening Methods, Tests Used, and What Women Can Expect
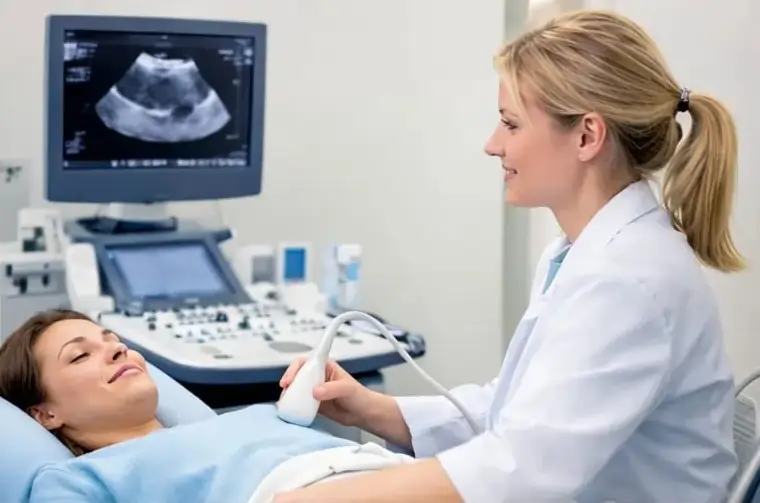
Once women understand the importance of gynaecological Cancer screening, the next natural question is how screening is actually done. Many women feel anxious because they are unsure about the tests involved or what the screening process looks like. Understanding the methods used in gynaecological Cancer screening helps reduce fear and prepares women to approach screening with confidence.
Screening methods vary depending on the type of Gynaecological Cancer being evaluated, a woman’s age, symptoms, and individual risk factors.
Common Screening Tests Used in Gynaecological Cancer Screening
Gynaecological Cancer screening does not rely on a single test. Instead, it uses a combination of evaluations to build a clear clinical picture. Each test has a specific role and purpose.
Pap Smear Test- Cervical Cancer Screening
The Pap smear is one of the most widely used and effective screening tests for cervical Cancer. It helps detect abnormal changes in cervical cells before they develop into Cancer.
During the test, cells are gently collected from the cervix and examined under a microscope. The procedure is quick and usually causes only mild discomfort. Regular Pap smears have significantly reduced the incidence of advanced cervical Cancer worldwide.
Pap smear screening is generally recommended for women above a certain age or based on individual medical advice.
HPV Testing and Its Role in Screening
Human papillomavirus (HPV) infection is a major risk factor for cervical Cancer. HPV testing identifies high-risk virus strains that are associated with abnormal cervical cell changes.
HPV testing may be done alone or alongside a Pap smear, depending on age and screening guidelines. A positive HPV test does not mean Cancer is present, but it signals the need for closer monitoring or further evaluation.
This test plays a key role in preventive Gynaecological care.
Transvaginal Ultrasound for Uterine and Ovarian Evaluation
A transvaginal ultrasound is commonly used to evaluate the uterus and ovaries. It provides detailed images of pelvic organs and helps identify structural abnormalities.
This test is especially useful for assessing uterine lining thickness, ovarian cysts, masses, or other changes that may require further evaluation. Ultrasound is non-invasive and does not involve radiation.
It is often used when women experience abnormal bleeding, pelvic pain, or unexplained symptoms.
Blood Tests Used in Gynaecological Cancer Screening
Certain blood tests may be included as part of screening or risk assessment, especially in specific age groups or clinical scenarios.
For example, CA-125 blood testing may be used in selected situations related to ovarian conditions. It is important to understand that blood tests alone do not diagnose Cancer. They are interpreted alongside imaging and clinical findings to guide further evaluation.
Doctors carefully decide when blood tests are appropriate to avoid unnecessary anxiety or misinterpretation.
Physical and Pelvic Examination
A pelvic examination remains an important part of Gynaecological Screening. During this examination, the doctor assesses the external and internal reproductive organs for any visible or palpable abnormalities.
Although it does not diagnose Cancer on its own, it provides valuable clinical information and helps determine whether additional tests are needed.
How Doctors Decide Which Screening Tests Are Needed
Not all women require all screening tests. Doctors recommend tests based on factors such as age, symptoms, menstrual history, family history, and previous screening results.
For example, a woman with no symptoms but above a certain age may need routine cervical screening, while someone with abnormal bleeding may require ultrasound and additional evaluation.
This personalised approach ensures accurate screening without unnecessary procedures.
What to Expect During a Gynaecological Cancer Screening Visit
A typical screening visit begins with a detailed discussion about medical history and current concerns. This is followed by physical examination and recommended tests.
Most screening procedures are completed on an outpatient basis and do not require hospital admission. Women are encouraged to ask questions and share any discomfort or concerns during the visit.
Clear communication is a key part of effective screening.
Understanding Screening Results
Receiving screening results can be stressful for many women. It is important to know that abnormal screening results do not automatically mean Cancer.
In many cases, abnormal findings indicate changes that need monitoring or further testing. Doctors explain results clearly and guide patients through the next steps if additional evaluation is required.
Importance of Follow-Up After Screening
Follow-up is an essential part of Gynae Cancer screening. Whether results are normal or abnormal, timely follow-up ensures continuity of care.
Women should always attend recommended follow-up visits and discuss any new symptoms, even if initial screening was normal.
Addressing Common Fears About Screening
Fear of discomfort, embarrassment, or results often prevents women from undergoing screening. Understanding that screening tests are generally quick, safe, and focused on prevention helps reduce these fears.
Healthcare providers aim to create a respectful and supportive environment to ensure patient comfort and privacy.
Age-Wise Screening, High-Risk Women, Prevention,
After understanding screening methods and tests, the most important question many women ask is “When should I start screening and how often should it be done?” The answer depends on age, individual risk factors, and overall health. Gynaecological Cancer screening is not a one-time activity but a continuous process that evolves with different stages of a woman’s life.
This section explains age-wise screening recommendations, screening for high-risk women, the role of lifestyle and prevention, and answers the most common questions women search online.
Age-Wise Approach to Gynaecological Cancer Screening
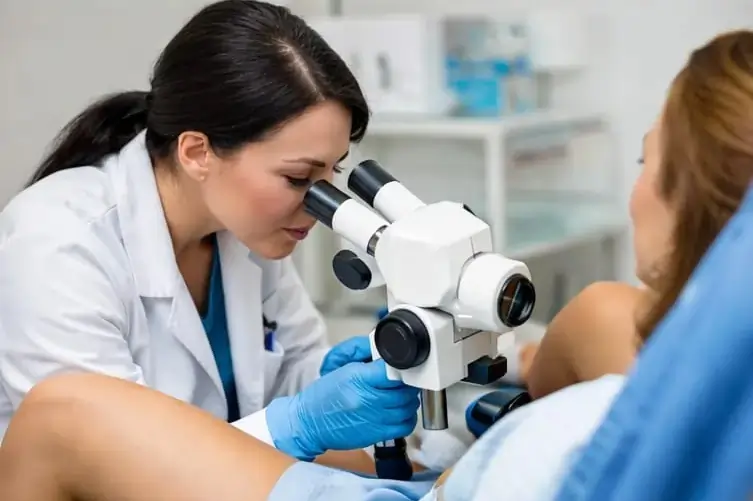
Screening needs change as a woman grows older. What is appropriate at one age may not be necessary at another. Doctors design screening schedules based on scientific evidence and individual health profiles.
Screening in Women Below 30 Years
In younger women, routine screening is usually focused on cervical health, especially if they are sexually active. Many gynaecological Cancers are rare in this age group, so screening is often symptom-based rather than routine.
If symptoms such as irregular bleeding, pelvic pain, or abnormal discharge occur, evaluation is recommended regardless of age.
Screening in Women Above 30 Years
Women above 30 are encouraged to be more regular with gynaecological Cancer screening. This age group benefits most from structured cervical screening and risk-based evaluation for other gynaecological Cancers.
Regular screening at this stage helps detect early cellular changes before symptoms appear, making it a critical phase for preventive care.
Screening After Menopause
Post-menopausal women require special attention because the risk profile changes after menopause. Abnormal bleeding after menopause is never considered normal and always needs evaluation.
Screening in this phase focuses on identifying uterine and ovarian abnormalities early, even if symptoms are mild.
How Often Should Gynaecological Cancer Screening Be Done?
The frequency of screening depends on the type of test and individual risk factors. Some tests are recommended at regular intervals, while others are done only when clinically indicated.
Doctors consider:
- Age
- Previous screening results
- Family history
- Hormonal status
- Presence of symptoms
Following recommended screening intervals helps balance early detection with avoiding unnecessary tests.
Screening for High-Risk Women
Some women have a higher risk of developing gynaecological Cancers and may need closer monitoring. High-risk factors include a strong family history of Cancer, genetic predisposition, long-term hormonal imbalance, obesity, or certain lifestyle factors.
For these women, screening may start earlier or be done more frequently. Individualised screening plans help ensure timely detection and appropriate follow-up.
Role of Lifestyle in Prevention and Early Detection
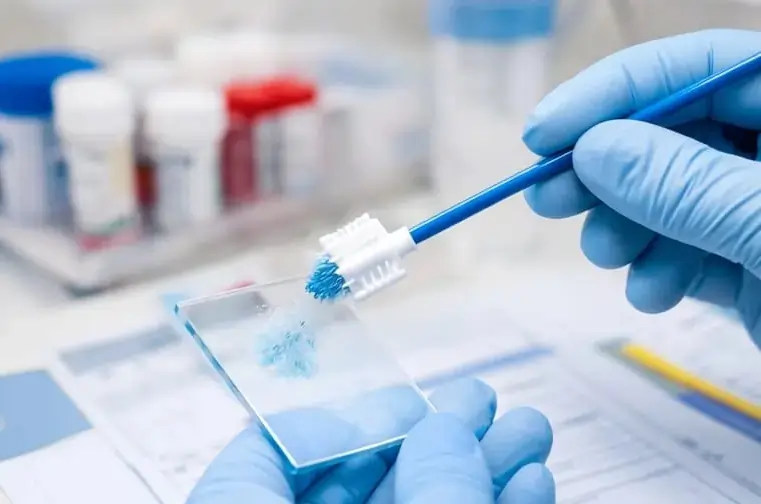
While screening plays a major role in early detection, lifestyle choices also influence long-term gynaecological health. Maintaining a healthy weight, staying physically active, and avoiding smoking can reduce certain Cancer risks.
Regular health check-ups and being attentive to bodily changes allow women to seek medical advice early, even between scheduled screenings.
Importance of Awareness and Self-Monitoring
Screening does not replace awareness. Women should remain alert to symptoms such as abnormal bleeding, persistent pelvic pain, bloating, or unexplained weight changes.
Self-monitoring combined with regular screening creates a strong foundation for preventive health care.
Emotional and Psychological Aspects of Screening
Fear and anxiety often prevent women from undergoing screening. Concerns about discomfort, results, or social stigma are common. Understanding that screening is a preventive step-not a diagnosis-can help reduce these fears.
A supportive healthcare environment and clear communication encourage women to participate in regular screening without hesitation.
FAQs – People Also Ask
When should women start gynaecological Cancer screening?
Screening usually begins in adulthood and becomes more structured after 30, based on individual risk factors.
Is gynaecological Cancer screening painful?
Most screening tests cause minimal discomfort and are well tolerated.
Can screening detect Cancer early?
Screening helps identify early changes that may require further evaluation.
Do women without symptoms need screening?
Yes, screening is often done even when no symptoms are present.
How long does a screening appointment take?
Most screening visits are completed within a short outpatient appointment.
What happens if screening results are abnormal?
Abnormal results usually lead to further tests, not an immediate diagnosis.
Is screening required after menopause?
Yes, especially if symptoms like bleeding occur after menopause.
Long-Term Benefits of Regular Gynaecological Cancer Screening
Women who follow recommended screening schedules benefit from:
- Early identification of abnormalities
- Reduced uncertainty about health
- Better planning of medical care
- Greater confidence in long-term well-being
Screening supports informed decision-making rather than reactive treatment.
Final Conclusion
Gynaecological Cancer screening is a vital component of women’s preventive healthcare. It empowers women to take control of their reproductive health by identifying potential concerns early, often before symptoms develop.
By understanding screening methods, following age-appropriate recommendations, and staying attentive to bodily changes, women can make proactive and confident health choices. Regular screening, combined with awareness and professional guidance, plays a key role in protecting long-term health and quality of life.
